
Back بروتيوباثي Arabic Proteinopati Danish Proteinfehlfaltungserkrankung German Protéinopathie French プロテオパチー Japanese Proteopatia Portuguese Протеинопатия Russian 蛋白质构象病 Chinese
| Proteinopathy | |
|---|---|
 | |
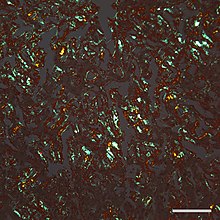
| Micrograph of a section of the cerebral cortex from a person with Alzheimer's disease, immunostained with an antibody to amyloid beta (brown), a protein fragment that accumulates in amyloid plaques and cerebral amyloid angiopathy. 10X microscope objective. |
In medicine, proteinopathy ([pref. protein]; -pathy [suff. disease]; proteinopathies pl.; proteinopathic adj), or proteopathy, protein conformational disorder, or protein misfolding disease, is a class of diseases in which certain proteins become structurally abnormal, and thereby disrupt the function of cells, tissues and organs of the body.[1][2] Often the proteins fail to fold into their normal configuration; in this misfolded state, the proteins can become toxic in some way (a toxic gain-of-function) or they can lose their normal function.[3] The proteinopathies include such diseases as Creutzfeldt–Jakob disease (and a variant associated with mad cow disease) and other prion diseases, Alzheimer's disease, Parkinson's disease, amyloidosis, multiple system atrophy, and a wide range of other disorders.[2][4][5][6][7][8] The term proteopathy was first proposed in 2000 by Lary Walker and Harry LeVine.[1]
The concept of proteopathy can trace its origins to the mid-19th century, when, in 1854, Rudolf Virchow coined the term amyloid ("starch-like") to describe a substance in cerebral corpora amylacea that exhibited a chemical reaction resembling that of cellulose. In 1859, Friedreich and Kekulé demonstrated that, rather than consisting of cellulose, "amyloid" actually is rich in protein.[9] Subsequent research has shown that many different proteins can form amyloid, and that all amyloids show birefringence in cross-polarized light after staining with the dye Congo red, as well as a fibrillar ultrastructure when viewed with an electron microscope.[9] However, some proteinaceous lesions lack birefringence and contain few or no classical amyloid fibrils, such as the diffuse deposits of amyloid beta (Aβ) protein in the brains of people with Alzheimer's.[10] Furthermore, evidence has emerged that small, non-fibrillar protein aggregates known as oligomers are toxic to the cells of an affected organ, and that amyloidogenic proteins in their fibrillar form may be relatively benign.[11][12]
- ^ a b Walker LC, LeVine H (2000). "The cerebral proteopathies". Neurobiology of Aging. 21 (4): 559–61. doi:10.1016/S0197-4580(00)00160-3. PMID 10924770. S2CID 54314137.
- ^ a b Walker LC, LeVine H (2000). "The cerebral proteopathies: neurodegenerative disorders of protein conformation and assembly". Molecular Neurobiology. 21 (1–2): 83–95. doi:10.1385/MN:21:1-2:083. PMID 11327151. S2CID 32618330.
- ^ Luheshi LM, Crowther DC, Dobson CM (February 2008). "Protein misfolding and disease: from the test tube to the organism". Current Opinion in Chemical Biology. 12 (1): 25–31. doi:10.1016/j.cbpa.2008.02.011. PMID 18295611.
- ^ Chiti F, Dobson CM (2006). "Protein misfolding, functional amyloid, and human disease". Annual Review of Biochemistry. 75 (1): 333–66. doi:10.1146/annurev.biochem.75.101304.123901. PMID 16756495. S2CID 23797549.
- ^ Carrell RW, Lomas DA (July 1997). "Conformational disease". Lancet. 350 (9071): 134–8. doi:10.1016/S0140-6736(97)02073-4. PMID 9228977. S2CID 39124185.
- ^ Westermark P, Benson MD, Buxbaum JN, Cohen AS, Frangione B, Ikeda S, Masters CL, Merlini G, Saraiva MJ, Sipe JD (September 2007). "A primer of amyloid nomenclature". Amyloid. 14 (3): 179–83. doi:10.1080/13506120701460923. PMID 17701465. S2CID 12480248.
- ^ Westermark GT, Fändrich M, Lundmark K, Westermark P (January 2018). "Noncerebral Amyloidoses: Aspects on Seeding, Cross-Seeding, and Transmission". Cold Spring Harbor Perspectives in Medicine. 8 (1): a024323. doi:10.1101/cshperspect.a024323. PMC 5749146. PMID 28108533.
- ^ Prusiner SB (2013). "Biology and genetics of prions causing neurodegeneration". Annual Review of Genetics. 47: 601–23. doi:10.1146/annurev-genet-110711-155524. PMC 4010318. PMID 24274755.
- ^ a b Sipe JD, Cohen AS (June 2000). "Review: history of the amyloid fibril". Journal of Structural Biology. 130 (2–3): 88–98. doi:10.1006/jsbi.2000.4221. PMID 10940217.
- ^ Wisniewski HM, Sadowski M, Jakubowska-Sadowska K, Tarnawski M, Wegiel J (July 1998). "Diffuse, lake-like amyloid-beta deposits in the parvopyramidal layer of the presubiculum in Alzheimer disease". Journal of Neuropathology and Experimental Neurology. 57 (7): 674–83. doi:10.1097/00005072-199807000-00004. PMID 9690671.
- ^ Glabe CG (April 2006). "Common mechanisms of amyloid oligomer pathogenesis in degenerative disease". Neurobiology of Aging. 27 (4): 570–5. doi:10.1016/j.neurobiolaging.2005.04.017. PMID 16481071. S2CID 32899741.
- ^ Gadad BS, Britton GB, Rao KS (2011). "Targeting oligomers in neurodegenerative disorders: lessons from α-synuclein, tau, and amyloid-β peptide". Journal of Alzheimer's Disease. 24 (Suppl 2): 223–32. doi:10.3233/JAD-2011-110182. PMID 21460436.